African Americans face more obstacles when battling coronavirus in Richland County
Midlands residents are impacted more by the coronavirus outbreak than those living elsewhere in the state, according to data provided by the S.C. Department of Health and Environmental Control.
African Americans of Richland County appear to be suffering the worst.
Despite being one of the later S.C. counties to report a COVID-19 case, Richland County’s case load has quickly ballooned above those in neighboring counties, as well as counties that are also densely populated. As of Friday, the county leads the state in both the number of confirmed cases (612) and deaths (14) and has the fifth-highest rate of infection based on its population size.
The reasons why are multi-faceted. Part of it is based in demographics.
African Americans comprise 48% of the county’s population and share similar disparities seen across the nation. National studies and census data show a disproportionate number of blacks in the U.S. live in poverty, resulting in less access to quality health care and higher rates of several health ailments, including heart disease, diabetes and hypertension, which increase susceptibility to coronavirus complications, officials say.
“It’s disturbing,” Columbia Mayor Steve Benjamin said. “Obviously, the issue around deaths and morbidity are enhanced by some significant systematic challenges that we face and discuss regularly.”
Geography plays a role in the reasons why, too.
Kershaw County, Richland’s neighbor, was the first to identify a coronavirus case, followed by a rapid increase in its case load. Benjamin suggested then that it was only a matter of time before Richland County was impacted.
Stay-at-home orders were not yet in effect and social distancing was not yet widely practiced.
Laura Renwick, a spokeswoman for DHEC, said it was expected for new cases to appear in the nearest area with a large population, which was Richland County.
“People travel across county lines frequently, and this disease doesn’t adhere to geographic boundaries,” Renwick wrote in an email. “Case rates can be influenced by numerous factors, and we expect those rates to fluctuate from day-to-day or across a period of time.”
While blacks make up approximately 27% of the state’s population, according to U.S. Census Bureau data, deaths due to complications from the coronavirus have disproportionately affected the African American community at an alarming rate.
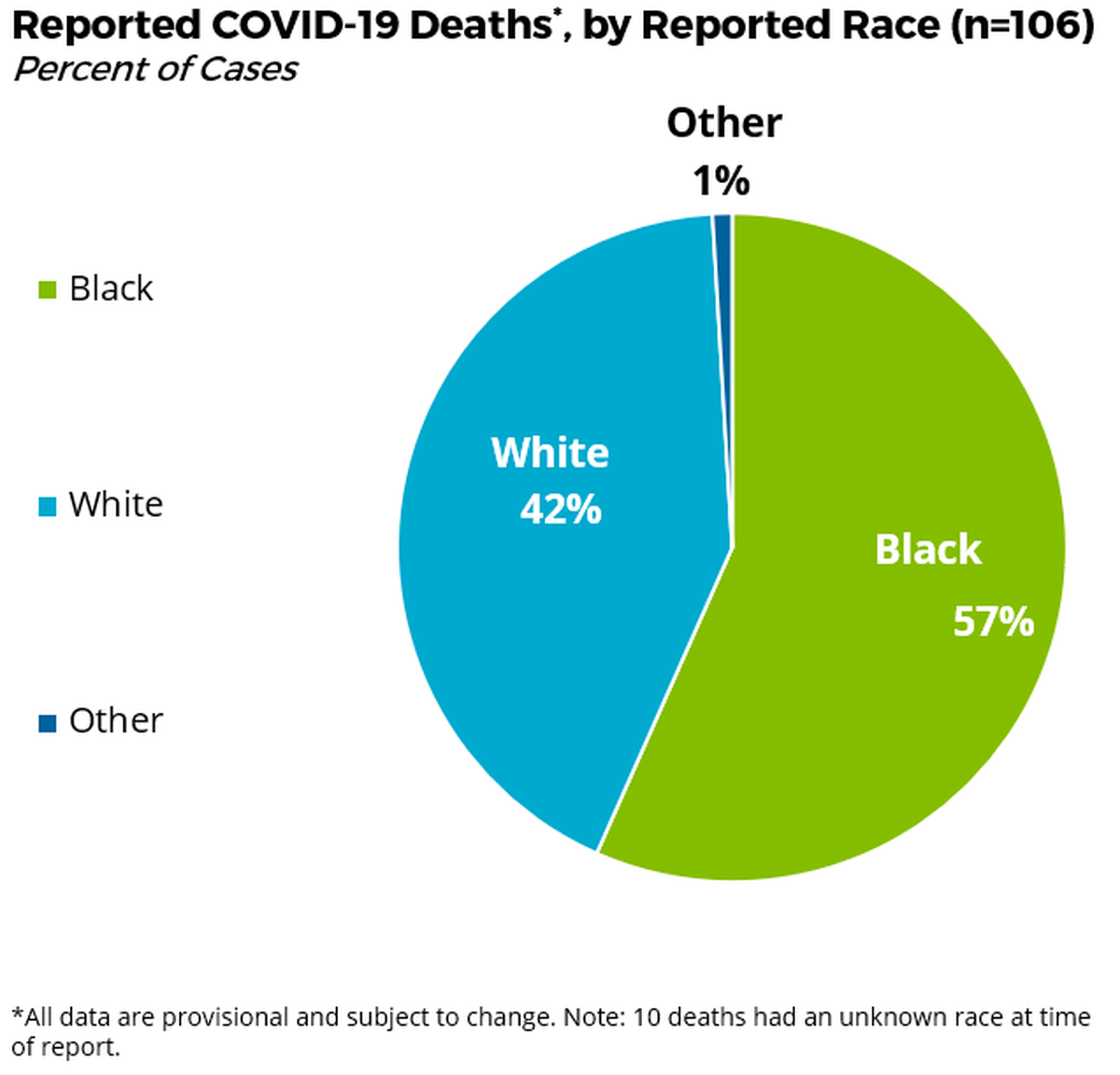
South Carolina has reported more than 4,000 cases of COVID-19. Of the 106 deaths for which race is known, 60 of those — or 57% — were blacks. While white people, who make up 68.5% of the population, account for 44 deaths —or 42% of the total. Another 10 additional deaths have been reported for which the race was not yet known.
Whites, however, make up 51% of the total coronavirus cases in South Carolina, while blacks make up just 41%. About 67% of patients have recovered.
About 90% of the deaths reported were patients ages 60 and older, though health officials warn that anyone can be affected due to how easily it can spread. DHEC has yet to release county-level data for patients based on age and race.
A majority of the region’s essential workers who don’t have the ability to work from home during the pandemic are also black, Benjamin said, which means they have a higher chance of contracting the virus and spreading it by interacting with others.
Benjamin said he has been studying how advances in automation and artificial intelligence will affect the workforce in the future and found that people of color will be impacted the most, adding that there is a significant overlap with essential jobs.
Transportation in Richland County is another obstacle blacks face during the pandemic.
Officials for the Midlands COMET bus system estimate that approximately 95% of its riders are black, the Free Times reported in January, placing people at risk of catching the virus while on their way to work or the grocery store for much-needed supplies and food.
House Rep. Wendy Brawley, D-Richland, said she thinks state leaders could be doing more to help the vulnerable population, particularly those living in rural parts of Richland County. She said obtaining basic county data from DHEC has been difficult and fears that testing isn’t being administered equitably across the region.
“We are not doing enough as a state to make sure we are taking care of the most needy population, and more often than not those are African Americans and Hispanics,” she said. “It’s as if the deck is stacked completely against you — and the state is closing their eyes.”
Rep. Todd Rutherford, D-Richland, said he, too, is concerned about testing and said he has been speaking with other lawmakers to help bring mobile testing into specific communities with higher rates of health complications. His hope is to eventually isolate people who test positive so they don’t go back to work or in a home with their loved ones and spread the virus.
“The tests are a lagging indicator and not indicative of where we really are,” he said.
Michael Sweat, director of the Medical University of South Carolina’s Center for Global Health and a professor of psychiatry and behavioral sciences, has been studying coronavirus data for months before it spread in the U.S.
He, too, said underlying health conditions and poverty play major roles in determining who is better off when contracting the virus. And someone’s income, he added, may prevent them from following health recommendations, such as obtaining a face mask or other supplies.
In Richland County, blacks make up 58% of those living in poverty, compared to just 27% of whites living in poverty.
“Every single one of those are major predictors of bad health outcomes,” he said. “And that is what predicts who’s going to get really sick and who’s going to die from that.”
Locally, it doesn’t take much more than a small social gathering, such as going to church, a birthday party or a funeral, for the novel virus to spread rapidly, Sweat said, which may have been what happened in Kershaw County.
In one tragic example, just weeks after a crowd gathered for a funeral in southern Kershaw County, six people who attended had died. All six were considered elderly — age 60 or older — and were African American, according to Sumter County Coroner Robbie Baker. A similar, but larger, event occurred in Albany, Georgia, that led to hundreds being infected in a county where blacks make up 70% of the population.
Sweat said the coronavirus has similarities to HIV and the flu, in terms of how rapidly it spreads and who it affects worse, but added that the novel virus is much more intense in how quickly it wears down the body.
Data suggests that a person with the flu infects around 1.3 people on average, he said, while the coronavirus is nearly double that with an average of 2.5 people. DHEC has shown projections that one person may infect roughly six to nine others due to delays of symptoms.
But the reasoning behind the spread of the virus differentiates based on location, Sweat added. And no one is immune.
“I think in an urban setting it has a lot to do with crowding, density of people living together. And the use of public transportation, you know, like in New York, people use the subway, and it’s very hard to separate yourself from people,” he said. “But when you get out in rural areas. I think you’re starting to tap in to a very dense, interconnected social network.”
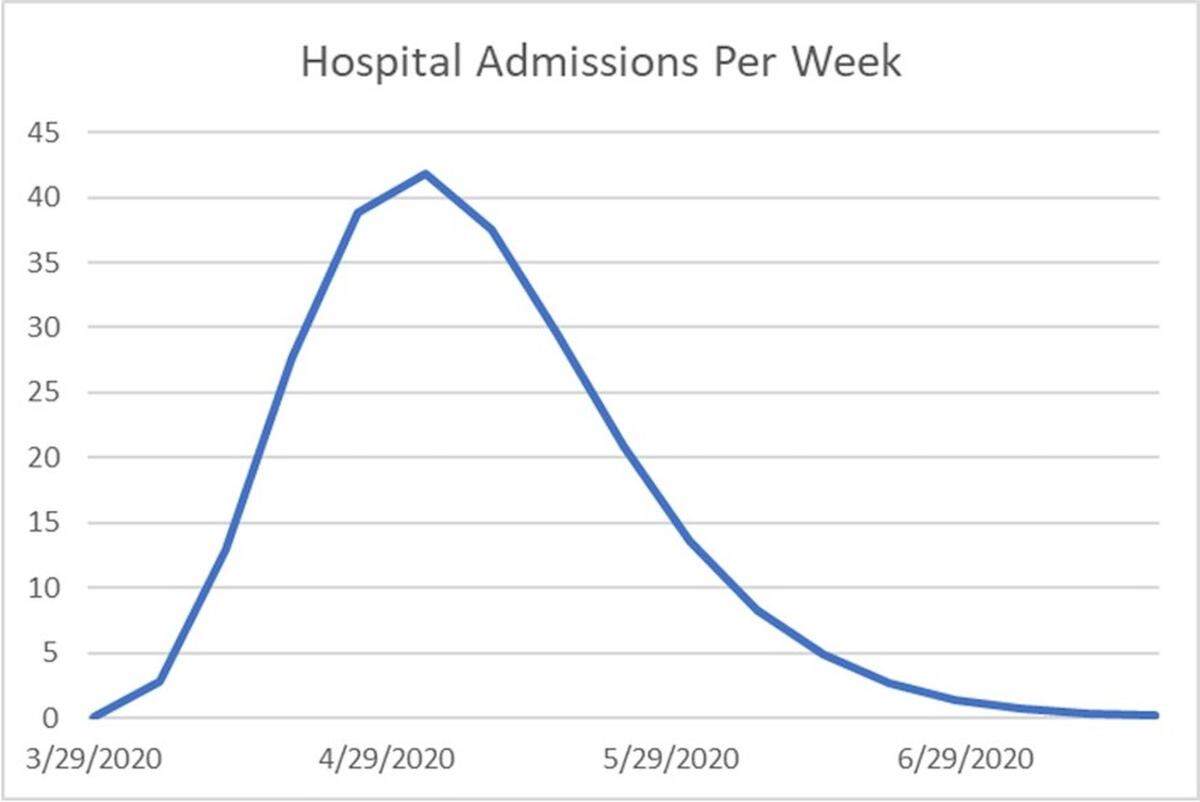
In the coming weeks, health officials are expecting to see another wave of cases around South Carolina. That’s largely due to symptoms not surfacing for up to two weeks.
As of Thursday, 343 patients were being treated for COVID-19 at facilities around the state, with about 5,500 empty beds. Rutherford said that for every 1,000 tests completed for the coronavirus, just six are hospitalized. For every six patients, he added, one ends up on a ventilator.
“The problem is a disproportionate number of those people are African Americans,” said Rutherford, who urged other lawmakers to take action. “If you ignore the (black) population this time, we will never be able to go back to normal.”
MUSC and other hospitals in the region have said they are prepared and have the capacity to handle the load, as long as people continue to follow guidelines from health professionals.
“The social distancing is working,” Sweat said. “It’s just painful. And it’s messing our economy up in an enormous way. I think the big challenge now is finding a way to unlock things and get back to more normal without having more and more waves of this until we can get to a vaccine.”
This story was originally published April 17, 2020 at 7:25 PM.