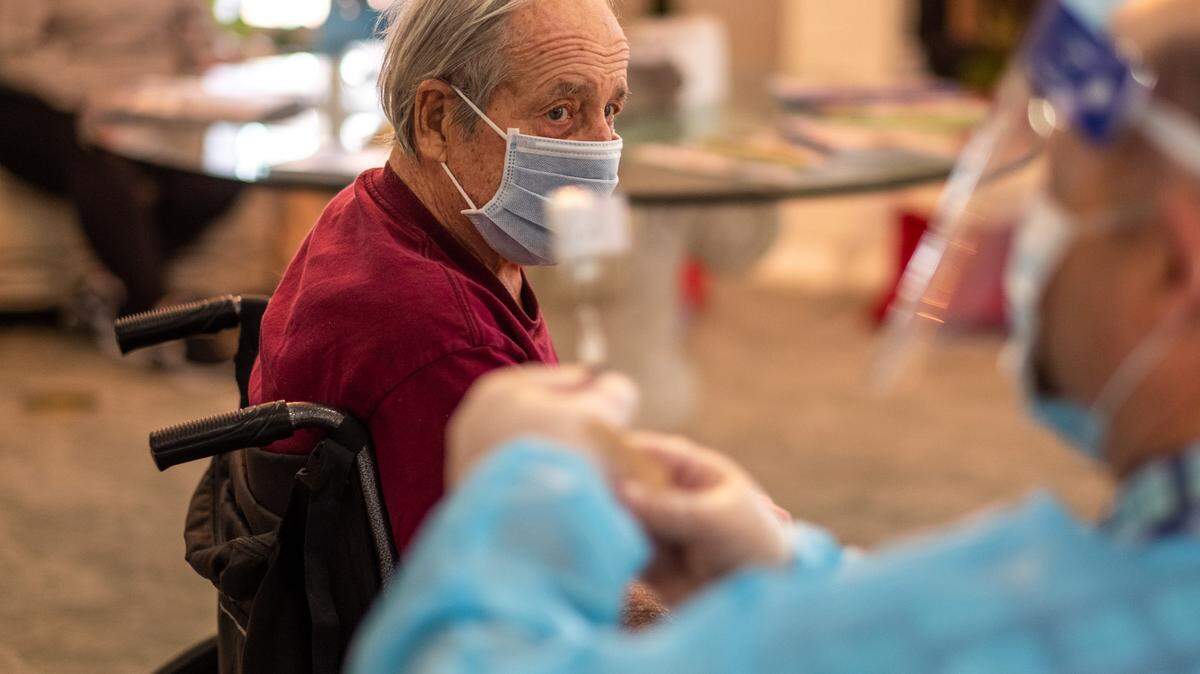
As delta surges, experts wonder whether SC will be ready for the next COVID variant
READ MORE
COVID-19 spikes again in South Carolina
Here’s the latest on the omicron variant surge, COVID-19 guidance and more in South Carolina.
Expand All
South Carolina’s COVID-19 case count is soaring and hospitalizations have surged sixfold over the past month as the highly contagious delta variant tears through the state’s large unvaccinated population.
The variant, which made up less than 1% of statewide cases in May, now accounts for an estimated 80% of new cases in South Carolina, according to the state Department of Health and Environmental Control.
Despite its presumed prevalence, state health officials can’t pinpoint the total number of delta cases in South Carolina or where in the state the variant is spreading in real time. As of Friday, DHEC had confirmed just 248 delta cases out of the many thousands the agency estimates South Carolinians have contracted in recent weeks.
That’s concerning, health experts say, because understanding how and where variants like delta are spreading has important clinical and public health implications. Health officials need to know what virus variants, if any, are circulating, to prepare targeted responses.
“That’s the point of public health,” said Dr. Julie Hirschhorn, director of the Medical University of South Carolina’s molecular pathology laboratory. “To be able to act as opposed to react.”
The relatively small number of delta cases confirmed in South Carolina reflects the fact that DHEC performs whole genome sequencing on only a tiny fraction of COVID-19 samples. Sequencing, which allows scientists to map out an organism’s genetic information, is crucial for identifying coronavirus mutants that may be more contagious, cause more severe disease or render vaccines or antibody treatments less effective.
Delta, first identified in India and now responsible for more than 93% of all COVID-19 cases nationwide, is one such mutant. The variant is more transmissible than SARS, MERS, Ebola, the 1918 Spanish flu, the common cold and even smallpox, DHEC medical consultant Jonathan Knoche said.
A number of studies have found that delta also may cause more severe disease than other COVID-19 strains — and there is a belief among some medical professionals that it hits younger, healthier people harder — but the case for delta’s increased virulence remains unsettled.
South Carolina health officials reported the state’s first delta case in late May, but it could have arrived here earlier and simply escaped detection because of how few coronavirus samples the state sequences.
Only 1% of all cases in South Carolina have been sequenced to date, according to the U.S. Centers for Disease Control and Prevention. GISAID, an international data sharing platform that hosts a global database of COVID-19 genomes, puts the number at 0.63%.
The U.S. in general sequences coronavirus cases at a far lower rate than many developed nations — it ranks 43rd in sequencing among countries with at least 100 COVID-19 infections, according to GISAID — but South Carolina’s rate is low, even for the U.S.
“We have no idea what’s actually happening, and I think that’s dangerous,” said Dr. Helmut Albrecht, director of the University of South Carolina’s Center for Infectious Disease Research and Policy. “It’s important to know where in this surge we are. We need this for planning, for our hospital capacity. We need this for which services we offer, when to stand up meetings. I think we take a lot of information out of this and I would like to have a better understanding where this is.”
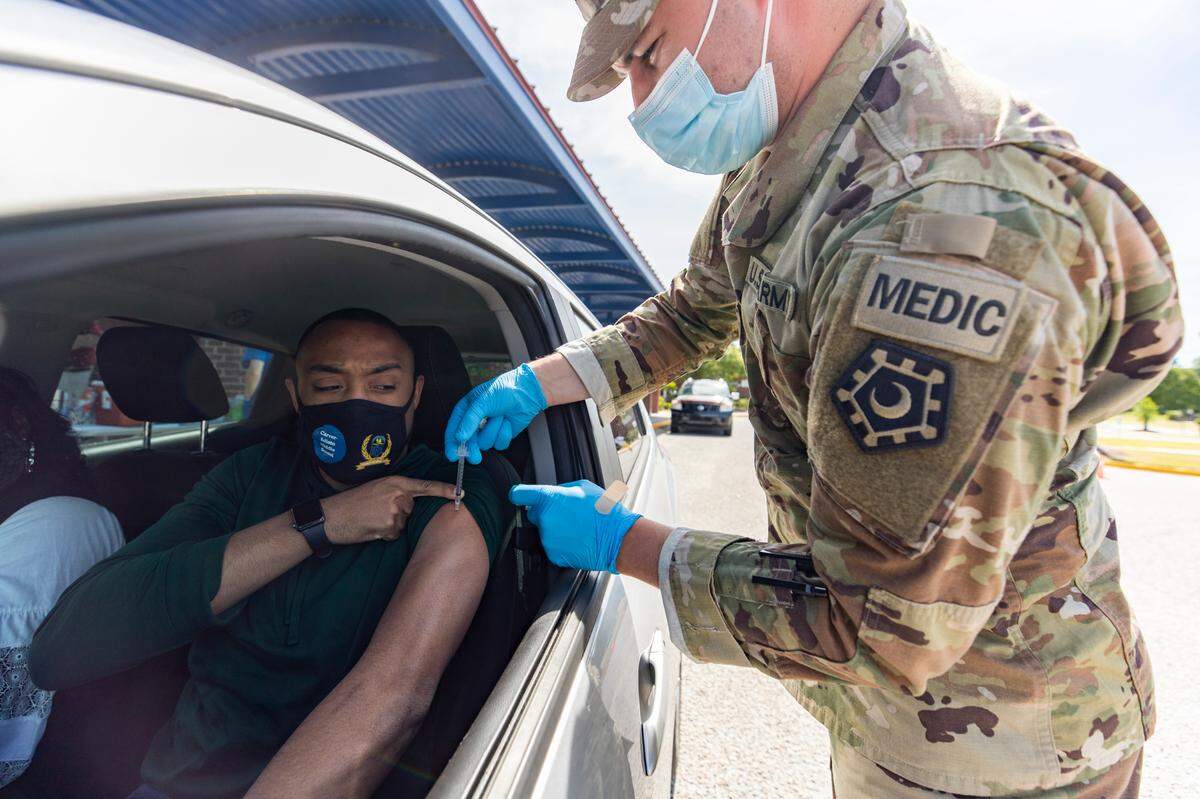
DHEC slow to ramp up sequencing
For months, the state health department has said it planned to ramp up sequencing efforts to better understand the spread of virus variants, but has shared scant details about those efforts.
In April, the agency launched what it said would be a two-week study to determine the prevalence of COVID-19 variants in the state, but four months later has yet to report that data on its website.
When asked recently about the delay, an agency spokesman said DHEC was still working to ensure the data was accurate and representative.
State health officials sporadically report how many COVID-19 samples its public health laboratory has sequenced, the percentage of those samples that are variants and the percentage of those variants that are delta, but have not provided a comprehensive variant breakdown upon request.
The agency’s online variant dashboard shows only the total number of each variant that has been identified in South Carolina, but not when they were found or their current prevalence.
The state lab sequenced 195 COVID-19 samples in June and 74 cases through the first two weeks of July, health officials said. DHEC tweeted this week that the delta variant now made up more than 80% of the state’s cases, but did not specify how many samples it had sequenced to reach that conclusion.
Spokesman Ron Aiken said Friday that the state lab has started sequencing 48 samples a day recently, as the number of positive cases has surged by an order of magnitude. That’s up significantly from the 24 samples a week it was sequencing earlier this year, but still only represents 1% to 2% of all daily cases.
The health department sequences samples submitted to the public health lab from all four regions of the state as well as samples it receives from other laboratories identified as vaccine breakthrough cases that resulted in hospitalization or death, Aiken said.
In addition to DHEC, the CDC and about a dozen private labs also sequence coronavirus samples in South Carolina.
Communication between the parties has been minimal throughout the pandemic and there exists no centralized repository of state sequencing data, although health officials are hoping to change that by developing a more comprehensive archive of sequencing data.
“There’s not really a good effort to capture all of the sequencing going on in the state,” said Hirschhorn, whose lab at MUSC sequences nearly 400 coronavirus samples every two weeks. “I’m not super familiar with any other locations that are doing sequencing outside of DHEC.”
The lab at USC’s School of Pharmacy also has sequenced hundreds of COVID-19 samples over the past couple months, but has no simple, automated way to share its data with DHEC, Albrecht said.
“There’s no good system in the U.S. set up for the CDC, and then therefore for DHEC, to submit sequences,” he said. “So we tell them, ‘Hey, we had an outbreak, they’re all delta,’ but there’s actually no way for us to submit the exact sequence, which, to us, means something.”
In June, the state health department began asking private labs to report their whole genome sequencing results and analyses within 24 hours of completion.
“Information collected from (whole genome sequencing) from across the United States and across the world can help determine where new variants may be emerging and if those variants show different dynamics from other variants,” Aiken said.
DHEC has since received sequencing data from at least eight labs, and two others, including Hirschhorn’s lab at MUSC, are working to sync up their systems with the state.
Health officials didn’t explain why they only began attempting to coordinate data sharing with outside labs in June, more than 16 months into the pandemic and a year after they began sequencing COVID-19 samples at the public health lab.
How will SC fare against the next novel variant?
Researchers like Hirschhorn, who said DHEC wasn’t initially responsive when her lab contacted the agency about sharing sequencing data some months back, believes the state’s recent interest in collecting this data is an important step in the right direction.
Sequencing will become increasingly critical to the state’s pandemic response in the months ahead, she said, especially as more people are infected with COVID-19 and the virus continues to replicate, because at some point a variant might emerge that is not just more transmissible but also impacts patient care.
“Over time, we could end up with a mutation that might prevent a vaccine from working or it may prevent one of the drugs that we use to treat COVID from working,” Hirschhorn said. “And then that would put us in a pretty bad position.”
Studies show that COVID-19 vaccines may be slightly less protective against delta, but all three vaccines available in the U.S. are still considered safe and highly effective against the variant when administered in full. People who are only partially vaccinated, meaning they’ve gotten only a single dose of the Pfizer-BioNTech or Moderna vaccines, fare significantly worse against delta.
Certain monoclonal antibody treatments, which are used to treat COVID-19 patients with minor symptoms and can prevent the disease from progressing and resulting in hospitalization or death, are also less effective, or in some cases ineffective, against virus variants, including delta.
Others remain effective against variants like delta, but less so.
That could change, however, and quickly.
“When we get to delta-plus, my suspicion is that we will see a significant drop off also of the other available antibodies,” he said. “Because there’s so many mutations in the spike protein that (the antibody treatments) were designed for that they probably don’t work anymore.”
Delta-plus is not necessarily fitter or more transmissible than delta — it might actually be less so — Albrecht said, but it has two mutations that make vaccines and therapeutic antibody cocktails less effective than they are against delta.
“We’re seeing right now only delta exploding, we’re not seeing delta-plus exploding,” he said. “But delta-plus is everywhere, lambda is everywhere, people are just not realizing that these viruses are everywhere.”
Delta-plus has not yet been identified in South Carolina, as far as Albrecht is aware, and even if it were here it may not cause a major problem. But the possibility that delta-plus or another novel variant could emerge in South Carolina speaks to the need for more genomic sequencing, experts say.
“The more sequencing that you do, the more likely you are to find novel variants, and those novel variants are gonna be the ones that could potentially have an impact on vaccine efficacy or transmissibility or monoclonal antibody treatments,” Hirschhorn said.
If South Carolina can get a head start on identifying and tracing the spread of the next concerning variant, the state and its medical institutions will be better able to prepare and effectively respond, experts say.
“We need to know this before it comes. Not when it’s 50% (of COVID-19 cases), right?” Albrecht said. “Then the horse is out of the barn.”
This story was originally published August 8, 2021 at 5:00 AM.













%20(5).jpeg)